Brief description
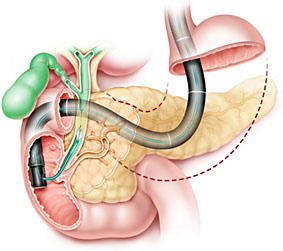
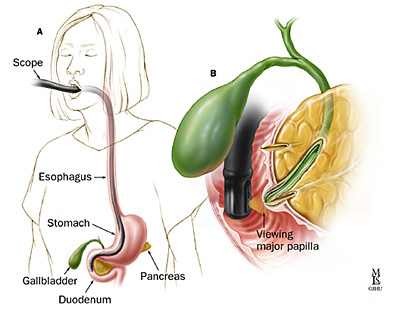
Your symptoms, blood tests and scans point to your gallbladder and bile ducts or pancreas being the cause of your symptoms. ERCP involves passing a flexible telescope (duodenoscope) through the mouth into and through the stomach to the first part of the bowel called the duodenum. Looking through this scope the outlet of the ducts (pipes) from the liver and pancreas can be seen. A small tube is then passed into these ducts. Contrast (dye) is injected and x ray films are taken. The x rays may show gallstones in the ducts or narrowing of the ducts. The tiny muscle at the bottom of the ducts is cut to create more space. Stones can then be removed, or small plastic tubes placed. This allows bile to drain out and into the bowel as normal.
Why is this operation necessary?
Blockage of the bile duct results in jaundice, and also often in infection. Relief of this blockage allows the bile to drain and the symptoms to resolve. Any gallstones within the ducts will be removed if possible. This procedure should only be performed if some type of intervention is required such as removal of stones, placement of stents etc. Due to the risk of the procedure, it should not be done solely for diagnostic purposes.
Are there alternative treatments available?
The alternative is open surgery to the bile duct. This is a major operation undertaken through a large abdominal incision (cut in the tummy). A successful ercp means that a much lesser operation can be performed later on to remove the gallbladder if required. If the ercp is being performed only to obtain information on the bile and pancreatic ducts then an mri scan with mrcp visualisation of the ducts is preferred to ercp as it is safer and provides the required information in most cases.
Is it safe to have this operation?
Before you agree to the operation, you should consider the risks that may be involved. Your procedure will be performed by a team of highly qualified and skilled professionals who will take all steps necessary to ensure a safe procedure and a successful result. However, there are risks involved with all procedures, even if these risks may be small.
WHAT ARE THE GENERAL RISKS INVOLVED?
There are risks for developing complications which are general and which may occur with any procedure. These complications include the risk of infection, bleeding, pain, deep vein thrombosis, or complications affecting the heart, lungs or kidneys.
WHAT ARE THE SPECIFIC RISKS INVOLVED?
Complications of some sort occur in up to 5% of people. Inflammation of the pancreas (pancreatitis), bleeding from the bile duct, infection of the bile, and perforation of the bowel may all occur. Usually these complications settle with treatment, although they require a prolonged hospital stay. In less than 1% of cases complications can be fatal.
WHAT ARE THE ANAESTHETIC RISKS INVOLVED?
You can discuss the type of anaesthetic you will have with your anaesthetist and also the possible complications that may occur. A heavy sedative is given, rather than a full anaesthetic. This means that you will still be breathing yourself, but you will be aware of little or nothing during the procedure.
WHAT SHOULD I DO BEFORE THE OPERATION?
You should not eat or drink anything for at least six hours before your ercp. However, you should take all your regular medication as usual on the day. You should stop certain medication such as disprin, warfarin, or other blood thinning medicines before the operation.
WHAT HAPPENS BEFORE THE OPERATION?
Please report to the hospital reception on time for your admission. Please bring along all the documents that may be required such as your medical aid card, id and con tact details. If you are not a member of a medical aid you will be required to pay a deposit or to sign an indemnity form. As far as possible we will try to advise you about hospital costs before your admission. It may be best to complete some of the documentation beforehand at the hospital pre-admission clinic to save time on the day of your admission.
When you arrive in the ward, you will be welcomed by the nurses or the receptionist and will have your details checked. Some basic tests will be done such as pulse, temperature, blood pressure and urine examination. You will be asked to hand in any medicines or drugs you may be taking, so that your drug treatment in hospital will be correct. Please tell the nurses of any allergies to drugs or dressings. The surgeon will have explained the procedure and you will be asked to sign your consent for the procedure. If you are not clear about any part of the procedure, ask for more details from the surgeon or from the nurses.
The anaesthetist who will be giving your anaesthetic will interview and examine you and he may put up a drip or prescribe some medication to help you relax. You will be taken on a trolley to the operating suite by the staff. You will be wearing a cotton gown. Wedding rings will be fastened with tape and removable dentures will be left on the ward. There will be several checks on your details on the way to the operating theatre where your anaesthetic will begin.
HOW LONG DOES THE OPERATION TAKE?
Around 45 minutes to an hour
WHAT HAPPENS WHEN I WAKE UP?
You will wake in the recovery area. You will remain drowsy for a time, and may only wake fully once back in the ward.
WILL I HAVE PAIN?
You may have some discomfort in the throat, but shouldn’t have much pain from the procedure.
HOW SOON AFTER THE OPERATION CAN I EAT?
You can eat normally as soon as you have woken.
HOW SOON AFTER THE OPERATION CAN I GET OUT OF BED?
As soon as you have woken fully, around an hour after the procedure.
HOW LONG WILL I STAY IN THE HOSPITAL?
Usually overnight, but it may be longer if you have preceding infection, or develop any complications.
WHAT HAPPENS WHEN I AM DISCHARGED FROM THE WARD?
You will be reviewed by the doctor prior to discharge. The nursing staff will perform the necessary paperwork, and you will be given a prescription if there is any medication necessary. You will be given a card with a follow-up appointment date and time.
WHAT SHOULD I BE AWARE OF WHEN I GET HOME?
If you develop a fever and cold shivers (rigors) you should contact the doctor. If you see any blood in the stool or vomit, or develop black stools, you should contact the doctor. Any jaundice will settle slowly over a few days.
HOW SOON CAN I START EXERCISE?
24 Hours after the procedure.
HOW SOON CAN I DRIVE A CAR?
You cannot drive on the day of the procedure, but can resume driving the following day.
HOW LONG WILL I BE OFF WORK?
You will only require the day of the procedure and the day of hospital discharge off work. However, the illness which required the procedure to be performed may re quire a longer period off work.
WHAT ABOUT PAYMENT?
The procedure and its associated costs will have been discussed with you, and a quote provided. Where procedures need to be unexpectedly altered during the course of the procedure, the fee may change. Similarly, emergency procedures may incur an additional cost. Surgeons are highly trained, highly skilled professionals and throughout your care a member of the practice is available to attend to you 24 hours a day. In return we expect prompt payment of your account.